Regenerative aesthetic medicine continues to grow rapidly in 2026, with more clinics integrating platelet-based procedures into skin rejuvenation, hair restoration, microneedling, and post-procedure recovery treatments.
Among the most commonly used regenerative approaches today are PRP (Platelet-Rich Plasma) and PRF (Platelet-Rich Fibrin).
Although both treatments are derived from the patient’s own blood and rely on concentrated platelets and growth factors, they differ significantly in:
- Preparation method
- Centrifugation protocol
- Anticoagulant usage
- Growth factor release profile
- Injection consistency
- Clinical workflow
- Treatment applications
For aesthetic clinics, hair restoration centers, and regenerative medicine professionals, understanding these differences is important when selecting the most suitable protocol for different treatment goals.
In this guide, we compare PRP vs PRF in detail, including how they are prepared, where they are commonly used, and why many clinics now offer both depending on the procedure.
What Is PRP?
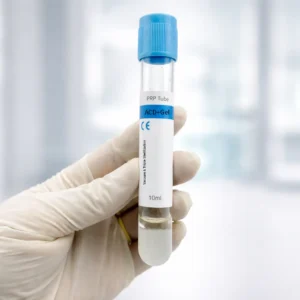
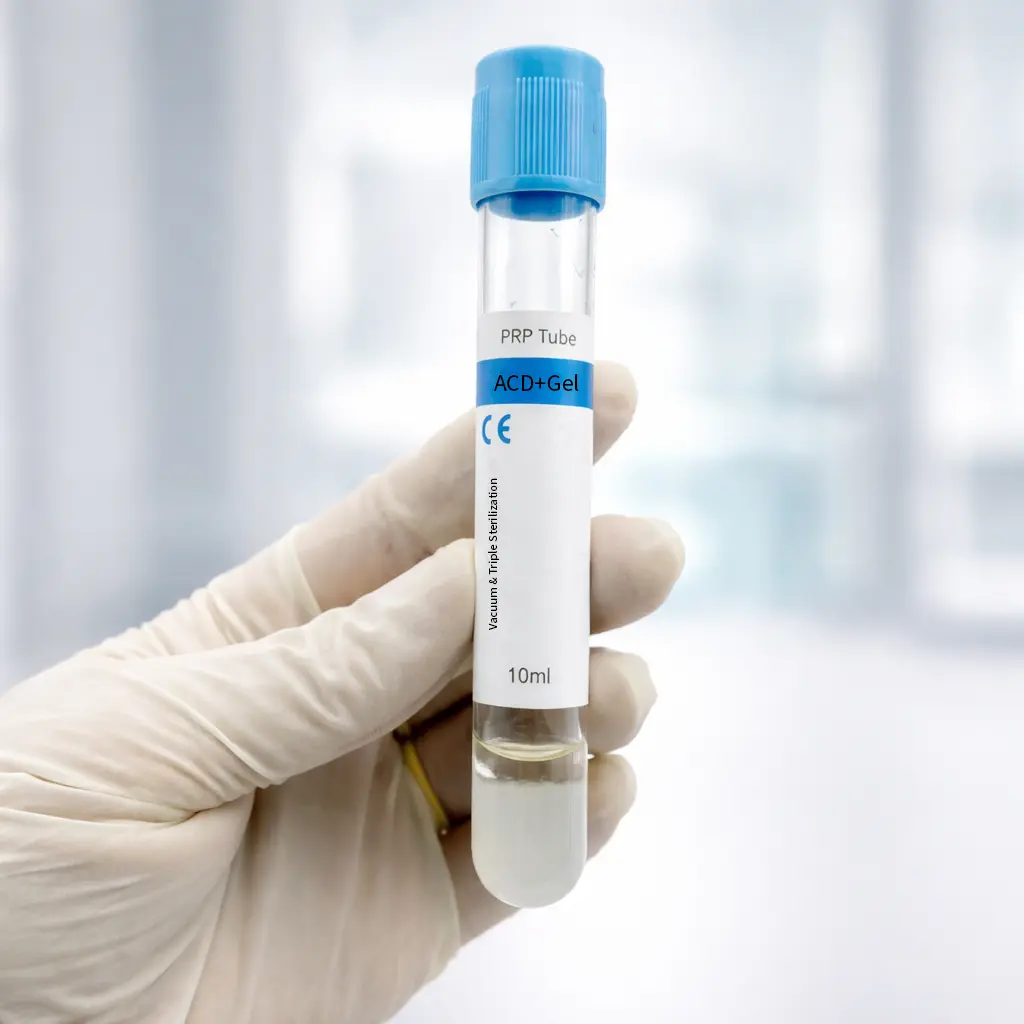
PRP (Platelet-Rich Plasma) is a concentrated plasma solution prepared by centrifuging the patient’s blood to separate and concentrate platelets from red blood cells. PRP tubes typically contain ACD-A anticoagulant and a separation gel. When centrifuged, red blood cells settle at the bottom, gel in the middle, and plasma on top. This plasma layer is then extracted for injection or topical use.
The resulting plasma contains:
- Concentrated platelets
- Growth factors
- Cytokines
- Plasma proteins
PRP has become widely used in:
- Hair restoration (androgenic alopecia)
- Facial rejuvenation (“PRP facials”)
- Microneedling treatments
- Dermatology procedures
- Orthopedic applications
- Sports medicine
In aesthetic medicine, PRP is often used to support skin rejuvenation and scalp treatment protocols by delivering concentrated platelets directly into targeted areas.
👉 Tube type: PRP tubes contain anticoagulant (ACD/sodium citrate) and a separating gel.
👉 Process: Blood is centrifuged to isolate platelet-rich plasma.
👉 Application: Injected into the target area or applied with microneedling.
What Is PRF?
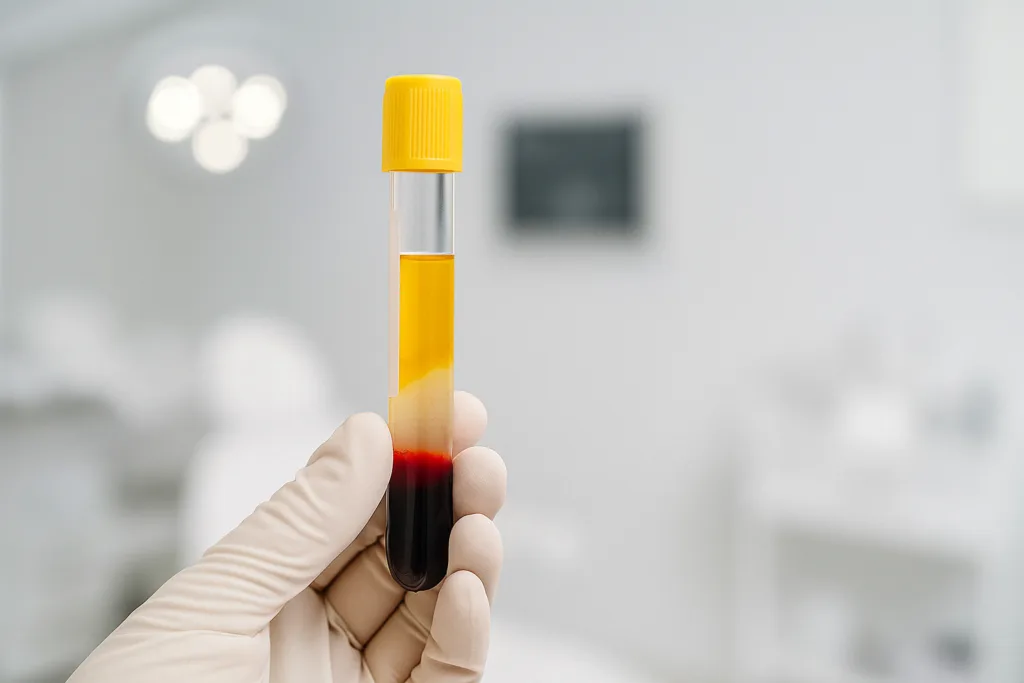
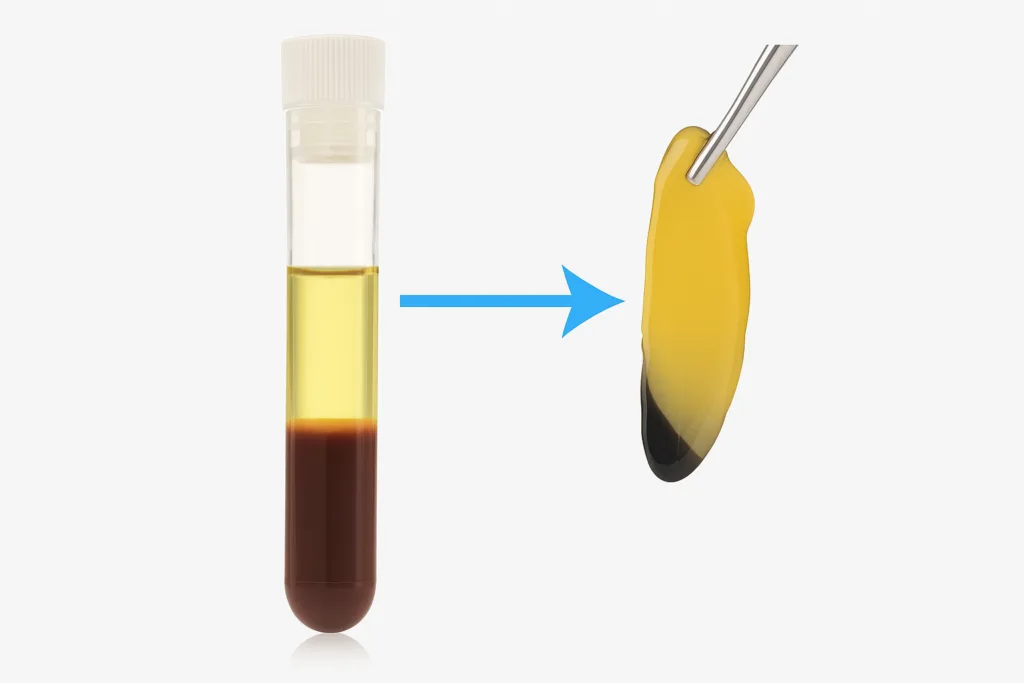
PRF (Platelet-Rich Fibrin) is often considered a second-generation platelet concentrate. Unlike traditional PRP, PRF is typically prepared without anticoagulants. During centrifugation, a fibrin matrix begins forming naturally, creating a more structured platelet concentrate.
The right choice depends on your treatment goals:
• For precision injections and hair restoration, PRP’s liquid form is ideal.
• For wound healing and dermal rejuvenation, PRF’s slow-release fibrin works better.
PRF commonly contains:
- Platelets
- Leukocytes
- Fibrin matrix
- Growth factors
PRF is increasingly used in:
- Under-eye rejuvenation
- Injectable regenerative treatments
- Hair restoration
- Facial volume-support procedures
- Dental and surgical healing applications
Because of the fibrin structure, PRF is commonly associated with slower and more sustained growth factor release compared to traditional PRP.
👉 Tube type: PRF tubes are additive-free (no anticoagulant). Some contain a natural gel separator.
👉 Process: Blood is centrifuged at higher g-force, forming a fibrin clot enriched with platelets and leukocytes.
👉 Application: Applied as a membrane or injected into treatment areas.

Key Differences in Preparation and Tubes
PRP vs PRF Comparison Table
The most defining difference between PRP and PRF lies in how they’re processed.
| Feature | PRP | PRF |
|---|---|---|
| Anticoagulant | Yes (usually ACD) | No |
| Tube Composition | Tube with ACD + gel | Plain glass or silica-coated tube |
| Centrifugation Speed | Higher speed (3,000–4,000 rpm) | Low speed (1,000–2,000 rpm) |
| Plasma Type | Liquid plasma | Fibrin clot |
| Growth Factor Release | Immediate | Sustained (up to 7–10 days) |
| Common Uses | Hair restoration, microneedling | Under-eye, regenerative aesthetics |
1. Anticoagulant Usage
PRP
PRP tubes typically contain anticoagulants such as ACD-A or sodium citrate to prevent clotting during centrifugation.
This helps maintain the plasma in liquid form for easier preparation and injection.
Many PRP tubes also include separation gel to support cleaner plasma isolation and more consistent layer separation.
PRF
PRF preparation generally avoids anticoagulants entirely.
Because clotting begins naturally after blood collection, PRF preparation requires faster handling and more precise timing during centrifugation.
This natural fibrin formation is one of the main characteristics distinguishing PRF from traditional PRP systems.
2. Centrifugation Protocol
PRP
PRP protocols commonly use:
- Higher centrifugation speeds
- Stronger centrifugal force
- Defined plasma separation layers
This helps isolate platelet-rich plasma efficiently while separating unwanted red blood cells.
PRF
PRF protocols generally rely on:
- Lower RPM
- Lower RCF
- Gentler centrifugation
Because clotting begins immediately, PRF processing is often more sensitive to timing and centrifuge configuration.
Why RCF Matters More Than RPM
One major mistake clinics make is relying only on RPM values when preparing PRP or PRF.
The more accurate measurement is RCF (Relative Centrifugal Force), since different centrifuges can produce different forces even at the same RPM.
The relationship between RPM and RCF is:
RCF=1.118×10−5×r×RPM2
Where:
- RCF = Relative Centrifugal Force
- r = rotor radius
- RPM = rotations per minute
This is why many manufacturers and clinics focus on target RCF values instead of RPM alone.
Different centrifuge rotor sizes can significantly affect platelet separation quality and treatment consistency.
3. Growth Factor Release
PRP
PRP is generally associated with faster growth factor release after injection.
This makes PRP highly popular for:
- Microneedling
- Scalp injections
- Facial rejuvenation
- Post-laser recovery support
PRF
PRF is commonly associated with slower and more sustained growth factor release because of the fibrin matrix structure.
This characteristic makes PRF increasingly popular for:
- Under-eye rejuvenation
- Injectable fibrin procedures
- Regenerative facial treatments
- Tissue-support applications
4. Injection Consistency
PRP
PRP remains liquid, making it easier to inject through smaller needles and mesotherapy systems.
This improves compatibility with:
- Automated injectors
- Microneedling procedures
- Scalp mesotherapy
- Combination aesthetic treatments
PRF
PRF has a thicker and more gel-like consistency due to fibrin formation.
Depending on preparation type, PRF may appear:
- Injectable
- Semi-solid
- Membrane-like
This affects both handling and injection technique.
The Science Behind Platelet Activation and Fibrin Formation
In PRP
ACD prevents clotting during preparation. Activation happens only when the PRP is injected into the tissue or combined with calcium chloride or thrombin. This gives practitioners precise control over when platelets start releasing their regenerative factors.
Key growth factors released include:
- PDGF (Platelet-Derived Growth Factor) – stimulates fibroblast proliferation
- TGF-β (Transforming Growth Factor Beta) – enhances collagen production
- VEGF (Vascular Endothelial Growth Factor) – promotes new blood vessel formation
In PRF
Because PRF contains no anticoagulant, clotting begins instantly. Platelets become embedded in a fibrin matrix, which acts as a scaffold that slowly releases growth factors over several days.
This sustained release mimics natural wound healing — ideal for tissue repair, bone regeneration, and post-surgical applications.
PRP vs PRF Tubes: Key Differences for Clinics
| Feature | PRP Tubes | PRF Tubes |
|---|---|---|
| Tube Composition | Contains anticoagulant (ACD/sodium citrate) + separating gel | No anticoagulant, natural clotting forms fibrin matrix |
| Platelet Concentration | Higher platelet concentration | Moderate platelet concentration, but includes leukocytes |
| Growth Factor Release | Fast release, strong initial effect | Slow, sustained release over several days |
| Centrifuge Protocol | Lower g-force (typically 1200–1500 RPM, 8–10 minutes) | Higher g-force (up to 2700 RPM, 10–12 minutes, depending on tube) |
| Composition | Platelet-rich plasma with minimal fibrin | Platelet-rich fibrin matrix with leukocytes & cytokines |
| Applications (Aesthetics) | Hair restoration, facial rejuvenation, scar treatment | Under-eye rejuvenation, skin tightening, wound healing |
| Safety & Naturalness | Anticoagulant needed, higher preparation control | More natural, additive-free, lower infection risk |
| Best For | High platelet demand (hair restoration, joint repair, aesthetics) | Long-term regeneration (dentistry, wound healing, facial PRF) |
Platelet Concentration and Biological Effects
Both PRP and PRF aim to concentrate platelets, but the method affects their distribution and functionality.
| Parameter | PRP | PRF |
|---|---|---|
| Platelet Concentration | 3–5× baseline | 2–3× baseline |
| Leukocytes | Variable | High |
| Fibrin Matrix | None (liquid) | Present |
| Growth Factor Release | Short burst (within hours) | Gradual release (up to 7 days) |
In essence, PRP = immediate boost, PRF = sustained healing.
Clinicians often combine both in comprehensive treatment plans — PRP for short-term rejuvenation and PRF for long-term tissue support.
Tube Composition: ACD, Gel, and Glass/PET
The choice of tube directly influences plasma purity and platelet recovery.
PRP Tubes
A quality PRP tube includes:
- ACD Anticoagulant: Prevents clotting, maintaining platelet integrity.
- Separation Gel: Ensures a clean plasma layer.
- Vacuum Sterility: Prevents contamination and air exposure.
This setup produces a clear, concentrated plasma layer ready for extraction. The separation gel barrier makes it ideal for hair restoration, facial rejuvenation, and intra-articular injections.
When PRP Is Preferred
Doctors often recommend PRP therapy when:
- High platelet concentration is needed quickly
- Treating sports injuries, joint conditions, or hair loss
- Performing cosmetic facial rejuvenation, scar treatment, or microneedling with PRP
- Patients require strong short-term healing response
PRF Tubes
PRF tubes are plain glass or silica-coated, without anticoagulant. The silica particles activate clotting, allowing the fibrin to form.
However, not all glass tubes are suitable for medical use. Clinics must ensure that their PRF tubes are CE certified and made from biocompatible borosilicate glass, as lower-quality tubes can cause cytotoxic reactions or unpredictable clot formation.
IPPOCARE offers both PRP tubes (ACD + Gel) and PRF tubes (no anticoagulant), allowing practitioners to select based on procedure type and patient profile.
When PRF Is Preferred
PRF may be more suitable when:
- A long-lasting regenerative effect is needed
- Performing oral surgery, implantology, or bone grafting
- Patients prefer a natural, anticoagulant-free preparation
- Treating chronic wounds or delicate under-eye rejuvenation
PRP vs PRF for Hair Restoration
Hair restoration clinics frequently use both PRP and PRF depending on treatment goals and practitioner preference.
Why Many Clinics Still Prefer PRP for Hair Restoration
PRP remains widely used because:
- Preparation is faster
- Workflow is easier to standardize
- Injection consistency is smoother
- It integrates easily with microneedling
- Most existing hair protocols are PRP-based
Many clinics also use specialized PRP tubes formulated for hair restoration procedures, including:
- Biotin PRP tubes
- HA PRP tubes
- ACD-A PRP tubes
Why Some Clinics Prefer PRF for Hair Treatments
PRF supporters often value:
- Fibrin-supported release
- Leukocyte inclusion
- Slower growth factor release
- Natural clotting process
However, PRF preparation is generally more time-sensitive and technique-dependent compared to PRP.
PRP vs PRF for Facial Rejuvenation
PRP in Facial Treatments
PRP is widely used with:
- Microneedling
- Fractional laser procedures
- Mesotherapy
- Acne scar treatments
- Skin rejuvenation protocols
Its liquid consistency makes it easy to combine with modern aesthetic devices and injection methods.
PRF in Regenerative Aesthetics
PRF has become increasingly popular in regenerative aesthetic procedures, especially for:
- Under-eye rejuvenation
- Tear trough support
- Injectable fibrin treatments
- Natural regenerative approaches
Some clinics prefer PRF for areas requiring slower-release regenerative support.
| Clinical Goal | Recommended Type |
|---|---|
| Fine-line reduction, glow, rejuvenation | PRP |
| Hair loss, scalp regeneration | PRP |
| Acne scars, wound healing | PRF |
| Bone grafts, oral surgery | PRF |
| Combined regenerative therapy | PRP + PRF hybrid |
Why Many Clinics Still Choose PRP in 2026
Despite growing PRF popularity, PRP remains the dominant platelet-based treatment in many aesthetic clinics worldwide.
1. Easier Workflow Integration
PRP protocols are generally:
- Faster
- More scalable
- Easier for staff training
- Less technique-sensitive
This is especially important for high-volume clinics.
2. Better Standardization
PRP systems often provide more consistent preparation workflows compared to PRF.
Because PRF begins clotting immediately after collection, timing variations can affect preparation quality.
3. Wider Equipment Compatibility
PRP systems are compatible with a broader range of:
- PRP tubes
- Centrifuges
- Injection systems
- Microneedling devices
4. Stronger Global Adoption
PRP remains more widely adopted globally across:
- Aesthetic clinics
- Hair restoration centers
- Dermatology practices
- Sports medicine clinics
This broader adoption contributes to easier workflow implementation and procedural familiarity.
Why PRF Continues Growing in Popularity
PRF continues gaining attention because many clinics are increasingly interested in:
- Natural regenerative procedures
- Lower-additive protocols
- Fibrin-supported treatments
- Sustained growth factor release profiles
Social media trends and regenerative aesthetics marketing have also contributed to increased PRF awareness in recent years.
Choosing the Right PRP or PRF Tubes
Both PRP and PRF therapies play important roles in regenerative medicine. The right choice depends on:
- Treatment goals (quick recovery vs sustained regeneration)
- Clinical specialty (aesthetics, dentistry, orthopedics)
- Patient preference (natural vs high-concentration therapy)
👉 At IPPOCARE, we provide a wide range of PRP tubes (Classic, Biotin, HA-enriched) and PRF tubes for doctors and clinics worldwide. Each tube is CE-certified, sterile, and optimized for platelet recovery to ensure safe and effective treatments.
| Factor | PRP | PRF |
|---|---|---|
| Preparation Time | 10–15 min | 5–8 min (must act fast) |
| Ease of Use | Easy to control | Time-sensitive |
| Consistency | Highly standardized | Variable (depends on timing) |
| Applications | Hair, face, joints | Wounds, bone, under-eye, scars |
| Additives Required | Anticoagulant (ACD) | None |
CE Certification and Safety Considerations
Regardless of whether you use PRP or PRF, tube certification is non-negotiable. The use of non-certified blood collection devices can result in contamination, inconsistent results, and regulatory violations.
CE-certified tubes ensure:
- Biocompatibility and sterility under ISO 13485 standards
- Proper vacuum calibration for exact blood volume
- Safe anticoagulant or activator dosage
Clinics should always verify documentation and choose suppliers with transparent testing data.
For reference, IPPOCARE’s Classic PRP Tube (ACD + Gel) and CE-certified PRP Tubes comply with ISO sterilization and quality requirements.
How Tube Choice Influences Results
The right tube design determines how many viable platelets and leukocytes are available for treatment.
- PRP tubes with ACD + gel ensure high yield and clean plasma.
- PRF tubes without additives ensure a natural fibrin network.
A substandard tube can trap platelets in the gel layer or trigger early clotting, wasting valuable plasma. Always use certified, medical-grade PRP and PRF tubes designed for clinical centrifugation.
PRP and PRF aren’t rivals — they’re complementary tools in regenerative medicine.
PRP offers precision and immediate biological activation; PRF provides structure and sustained healing. Together, they form a complete strategy for cellular repair, collagen remodeling, and long-term tissue health.
Understanding the science — and choosing the right CE-certified tube — allows clinics to achieve reproducible, high-quality outcomes for every patient.
- PRP provides high platelet concentration and rapid healing, making it ideal for aesthetics and sports medicine.
- PRF delivers a sustained, natural release of growth factors, making it valuable in dentistry, wound care, and delicate facial rejuvenation.
By stocking both tube types, clinics can provide customized treatment options that improve patient outcomes and build trust.
👉 Ready to equip your clinic?
Explore our full selection of PRP tubes and PRF tubes, CE-certified and trusted by aesthetic professionals worldwide.
🔗 Explore Related Products
PRF Tubes for Clinical Use
CE-Certified PRP Tubes
Classic PRP Tube (ACD + Gel)
FAQs About PRP and PRF Tubes
What is the main difference between PRP and PRF?
PRP uses an anticoagulant and remains in liquid form, while PRF is made without anticoagulant, forming a fibrin matrix for slow growth factor release.
Can PRP and PRF be used together?
Yes. Many clinics combine PRP and PRF to achieve both immediate and sustained regenerative effects.
Do PRP tubes always need anticoagulants?
Yes. PRP tubes contain ACD or sodium citrate to prevent clotting, allowing proper platelet separation during centrifugation.
Is PRF safer than PRP?
PRF is considered more natural since no anticoagulant is used, but both are safe when prepared with sterile, certified tubes.
Which is better for hair restoration, PRP or PRF?
PRP is generally preferred due to its higher platelet concentration, though PRF may be used for supportive regeneration.
How do I choose the right tube?
It depends on your specialty and patient needs. For facial aesthetics and hair restoration, PRP tubes (with or without HA) are ideal. For oral surgery and wound healing, PRF tubes are recommended.
What is the difference between PRP tubes with gel and without gel?
PRP tubes with a separating gel allow for clear plasma separation during centrifugation, resulting in higher platelet recovery and cleaner plasma for injections. Tubes without gel may lead to contamination with red or white blood cells, making them less suitable for consistent clinical use. Most modern PRP tubes for professional use include both gel and anticoagulant (ACD) for optimal platelet yield.
Are PRP and PRF tubes reusable?
No. PRP and PRF tubes are single-use, sterile medical devices. Reusing tubes increases the risk of infection and violates medical safety standards.
Always dispose of used tubes in a proper biohazard container according to hospital and clinic regulations.
How many milliliters should a PRP or PRF tube be?
PRP and PRF tubes are commonly available in 8mL, 10mL, or 12mL sizes. For facial treatments or small-area injections, 8-10mL tubes are usually sufficient. For hair restoration or orthopedic procedures, doctors often prefer 10-12mL tubes to ensure enough plasma volume is collected. The choice of tube size depends on the treatment area and required platelet concentration.
PRF is generally associated with slower and more sustained growth factor release due to the fibrin matrix structure.
📅 Last Updated: May 2026